Peripheral vision can be lost in the early stages of glaucoma. The loss of peripheral vision may be so subtle that the individual is not aware of this condition until late in the disease. For this reason, glaucoma is called “the silent thief of sight.” As the disease progresses, the loss of visual field can move away from the periphery toward the center of vision.
Classically, we say that glaucoma can cause “tunnel” vision. You can demonstrate this by closing one eye, and using the open eye to look through a tube such as the cardboard cylinder on the inside of a roll of aluminum foil. If you do this, you will notice that your vision straight ahead may be normal. You will also notice that you cannot see much above, below, or to either side of the object you are focusing on. This gradual loss of peripheral vision can become very disabling. Driving may become difficult due to an inability to detect cars on either side. Changing lanes and merging onto the highway become challenging tasks. Because the disease often progresses slowly, the person experiencing the visual field loss is rarely aware until quite late in the disease process.
3 Steps for Diagnosing Glaucoma
1. Intraocular Pressure
See our previous blog post on intraocular pressure.
2. The Visual Field Test
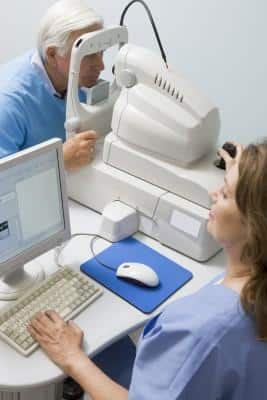
We can test peripheral vision using what we call a visual field machine or perimeter. This machine is basically a giant computer screen shaped like a large bowl. The patient is positioned so that their head is placed in the center of this bowl. One eye is patched closed. The other eye focuses on a target at the center of the bowl. Small lights are then flashed on the computer screen. The patient pushes a small hand-held button when he or she sees the flashing light. Using lights of varying size and intensity we can make an accurate map of the patients’ peripheral vision. The results of this test allow the doctor to judge the “health” of the optic nerve. This assessment is a vital piece of information in diagnosing glaucoma and following its course over time.
3. Evaluating the Optic Nerve and Nerve Fiber Layer
The first two pieces of information needed to make a diagnosis of glaucoma are the intraocular pressure and the visual field test. The third piece of information needed to make a diagnosis of glaucoma is the appearance of the optic nerve and the nerve fiber layer. There are many tools available to directly evaluate the optic nerve and nerve fiber layer. Images of the optic nerve are obtained with both a standard camera, as well as a laser imaging system. Baseline images should be obtained anytime glaucoma is suspected. As the patient is followed over time, repeat images are obtained and comparisons to the baseline studies are used to assess stability or progression of the disease.


