
Cornea
Our Arizona cornea specialists are highly trained in diagnosing and treating various corneal conditions, from dry eye and infections to complex surgical needs like corneal transplantation.
Overview of the Cornea
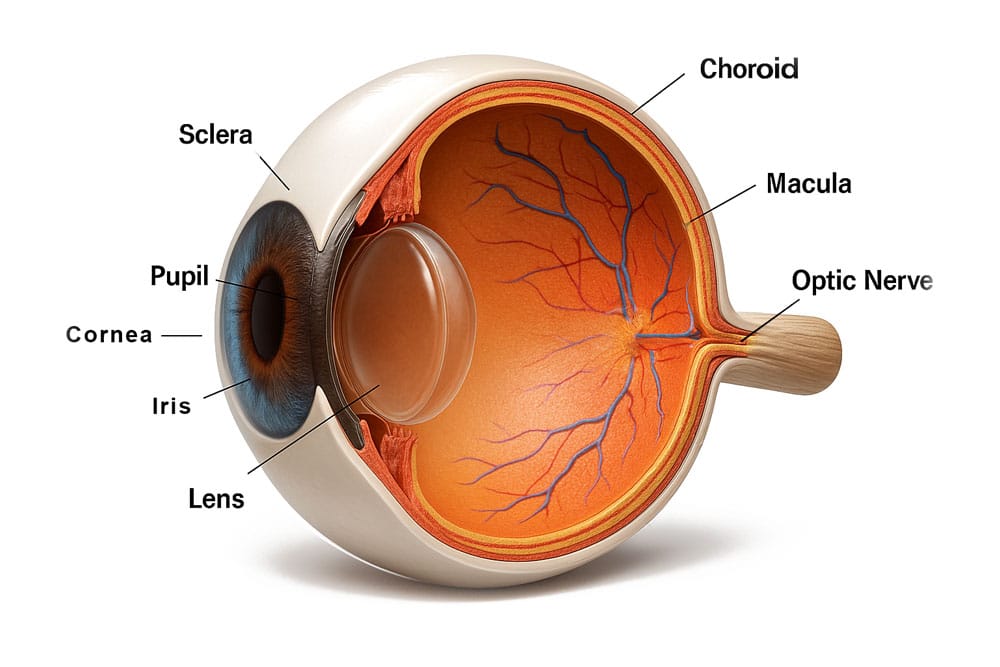
What is the Cornea?
The cornea is the clear, dome-shaped surface covering the eye’s front. As the first structure that light passes through, the cornea plays a crucial role in focusing vision, accounting for nearly two-thirds of the eye’s total focusing power. When the cornea is damaged by disease, injury, or age-related changes, it can significantly impact your vision.
Common Cornea Conditions We Treat
Dry Eye
Due to the desert environment here in Arizona, many people suffer from a feeling of eye dryness, or “dry eye.” Symptoms range from an irritated eye in certain conditions to blurriness, redness, and foreign body sensation. These symptoms may only mildly interfere with one’s life or in some cases cause a severe disability. This irritation of the surface of the eye can have many different causes and is important for us to determine which ones apply to you. A variety of treatment options are available, the choice of which depends on the severity of the disease and what is seen on examination.
Inflammation and Infection of the Conjunctiva and Cornea
The conjunctiva is a thin, transparent membrane covering the eye’s white part and the eyelids’ inside. Inflammation of the conjunctiva—commonly known as conjunctivitis—can result from allergies, chemical exposure, or infections. Infectious causes may include viruses, bacteria, fungi, or protozoa.
When an infection involves the cornea, the clear front surface of the eye, it can lead to a condition known as keratitis, which may result in a corneal ulcer. Symptoms of corneal infection often include eye redness, pain, sensitivity to light, and blurred or decreased vision. If left untreated, these infections can cause permanent scarring, which may significantly impair vision.
Prompt diagnosis and treatment are essential to prevent long-term damage. Common risk factors for corneal infections include contact lens wear, eye injuries, and trauma.
Keratoconus
Keratoconus is a common corneal condition in which the cornea begins to thin. As it thins, it loses strength, and aspects of the cornea start to bulge. The cornea changes into an abnormal shape, and one’s vision becomes affected. Initially, the vision can be corrected with glasses or contact lenses. As the disease progresses, there is loss of vision and corrective lenses may no longer be effective. It is recommended that patients with progressive keratoconus undergo early crosslinking treatment of the cornea to prevent progression of their disease and permanent vision loss. This treatment is performed in the office, and is the only FDA-approved treatment to halt the progression of keratoconus. Patients with severe untreated Keratoconus may need to undergo a full thickness corneal transplant in order to restore good vision.
Endothelial Keratoplasty (Partial corneal transplantation):
In patients who have corneal disease affecting the endothelium (the innermost layer of the cornea), partial corneal transplantation can be offered to restore vision. Two types of partial thickness corneal transplants offered are Descement’s Membrane Endothelial Keratoplasty (DMEK) and Descemet’s Stripping Automated Endothelial Keratoplasty (DSAEK). In these procedures, a smaller amount of corneal tissue is transplanted, offering faster visual recovery for patients with corneal swelling caused by endothelial conditions such as Fuchs’ dystrophy and endothelial damage. Only a very thin layer of cornea is removed and then replaced with a thin layer of donor cornea. Patients who undergo partial corneal transplantation also have better visual potential and a lower risk of rejection when compared to full thickness corneal transplants.
