
Macular Hole
A macular hole is a small opening in the macula, the part of your retina responsible for sharp central vision. Schedule a retina evaluation with us today to confirm the diagnosis and learn which treatment options can help protect your sight.

What is a Macular Hole?
A macular hole is a full-thickness opening in the macula, the central part of the retina responsible for sharp, straight-ahead vision. When the macula is disrupted, central vision can become blurry or wavy, and some people notice a dim or missing spot in the center of their vision, which can make reading, driving, and seeing fine detail harder.
Macular holes most often form when normal, age-related changes in the vitreous gel tug on the macula and create traction over time. If you notice new distortion, straight lines that look bent, or a sudden dark spot in your vision, it is worth getting evaluated quickly, as early care can improve outcomes. Treatment may include close monitoring for small cases or surgery to help the opening close and protect long-term vision.

Symptoms
Symptoms often start gradually, especially if the other eye still sees well, which can make changes easy to miss at first. Many people notice the problem most when reading, looking at phone screens, or focusing on fine detail, because a macular hole affects the center of vision more than peripheral vision.
Common symptoms include:
- Blurry central vision
- Distortion, straight lines look bent or wavy
- Difficulty reading small print or seeing fine details clearly
- A dark, blurry, or missing spot in the center of vision in more advanced cases
- Colors or contrast that seem slightly “off” in the affected eye
If you notice any of these changes, schedule an eye exam, especially if the symptoms are new or worsening and affect daily tasks like driving or reading.
Causes and Risk Factors
Age 55–60+
Normal aging changes in the vitreous gel can increase traction on the macula, making a macular hole more likely over time.
Being very nearsighted
High myopia can stretch and thin the retina, which may make the macula more vulnerable to traction and tissue changes.
Prior eye injury
Trauma can disrupt the vitreous or retina and trigger scarring or traction that increases the chance of a macular hole forming.
Prior eye surgery
Some surgeries can change how the vitreous sits or moves in the eye, which may increase macular traction in certain cases.
Inflammation inside the eye
Inflammation can lead to swelling and scar-like membranes on the retina, which can pull on the macula and contribute to a hole.
Diabetes and certain retinal conditions
Conditions that affect retinal health can increase the risk of macular traction or swelling, raising the chance of a macular hole in some settings.
How We Diagnose it
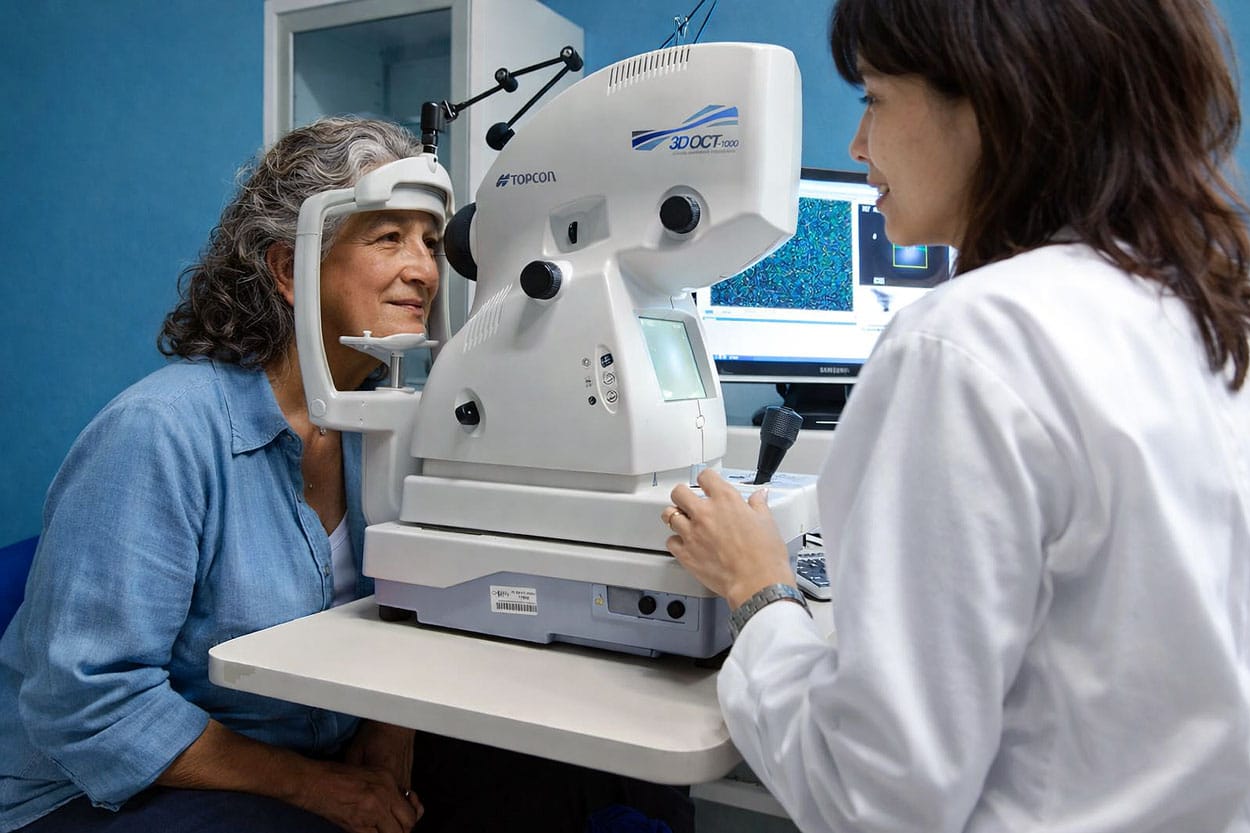
Diagnosis usually starts with a comprehensive dilated eye exam, followed by imaging to confirm the opening and determine the size and stage of the macular hole. Because symptoms can overlap with other retinal conditions, testing helps your retina specialist pinpoint the cause of your central vision changes and check for related findings that may affect treatment planning.
Common testing includes:
Optical coherence tomography (OCT): detailed cross-sectional retinal imaging that shows the macula in high detail, helping confirm a macular hole, measure its size, and track healing or changes over time.
Retinal evaluation after dilation: a close exam of the macula and the rest of the retina after dilation to look for traction, membranes, swelling, or other retinal issues that can contribute to symptoms or influence next steps.
Treatment Options
Treatment depends on size, symptoms, and whether the opening is stable or progressing.
Observation for small or early cases
Some small or early-stage macular holes may be monitored closely, especially if symptoms are mild.
Vitrectomy surgery
For many patients, the most common treatment is vitrectomy, in which the vitreous gel is removed to relieve traction, and a gas bubble is placed to gently press and support closure as the eye heals.
Your surgeon may also remove fine membranes that contribute to macular tension.

What to Expect with Surgery
Vitrectomy is typically performed by a retina specialist. During the procedure:
- The vitreous is removed
- Tissue on the surface of the macula may be addressed to reduce traction
- A gas bubble is placed to support healing
Many people are asked to maintain a specific position, sometimes face down, for a period of time, so the bubble stays in the correct place while the opening closes. The required duration varies based on the hole’s characteristics and the surgeon’s guidance.

Recovery and Aftercare
Recovery is not just about time; it is also about protecting the gas bubble’s position while healing happens.
What to expect during recovery:
- Vision is typically blurry while the gas bubble is present
- Activity limits are common, and positioning instructions may be required
- You must avoid flying and avoid nitrous oxide anesthesia until the bubble is fully gone because high eye pressure can become dangerous
Vision may continue improving for months after surgery, and your care team will guide follow-up visits and imaging to confirm healing.
Results and Outlook
Surgery outcomes are often strong, especially when the opening is smaller and treated earlier. Reported closure success rates for vitrectomy are commonly over 90%, with many patients regaining some or most of the vision they lost.

Risks and Possible Complications
All procedures carry risk. Potential complications discussed in reputable patient resources include:
- Cataract progression after retina surgery
- Retinal detachment
- Infection
- Glaucoma or elevated eye pressure
- Bleeding
- The hole is not closing or reopening in a minority of cases
Your surgeon will review your personal risk profile and what warning signs should prompt an urgent call.
When to Seek Urgent Care
Contact your eye care team promptly if you have severe eye pain, a sudden decrease in vision, or any sudden new flashes, floaters, or a curtain-like shadow in your vision, especially after a procedure.
FAQ: Macular Hole
What does a macular hole look like in my vision?
Many people notice distortion, straight lines look wavy, or a blurred or dark spot in the center of vision
Can a small macular hole heal without surgery?
Some small or early-stage cases may be observed, and in select situations, an early-stage opening may close on its own. Your doctor will guide the next steps based on OCT findings and symptoms.
How is a macular hole diagnosed?
A dilated eye exam plus OCT imaging is commonly used to confirm the diagnosis and guide treatment.
What surgery is used to treat it?
Vitrectomy is the most common surgical approach, often paired with a gas bubble to support closure while the eye heals.
Will I have to stay face-down after surgery?
Some patients are instructed to maintain face-down positioning for several days, and in some cases longer, depending on the characteristics of the opening and the surgeon’s plan.
Can I fly after surgery?
Not while the gas bubble is still present. Flying can change pressure in a way that raises eye pressure dangerously; your surgeon will tell you when it is safe.
