One of the most surprising things about cataracts is how quietly they affect your vision. The changes happen so gradually over the years that they’re easy to miss. Many people don’t realize how much cataracts have dulled their sight until after surgery, when bright whites, vivid colors, and crisp details come back into focus. Cataract surgery offers a chance to see the world again with clarity, brightness, and life.
A Closer Look at Your Eye
When you look in the mirror, you see the black center of your pupil, the colored ring of your iris, and the white of your eye. You don’t see the clear lens just behind the pupil and iris. This lens helps focus light onto the retina so the images you see can be sent to your brain.
A healthy lens is obvious, but over time, natural proteins inside the lens can clump together, forming cataracts. As the lens becomes cloudy, vision dims, colors fade, and details blur. A sky that once appeared bright blue may look dull, brownish, or hazy to someone with advanced cataracts.
Cataract surgery restores sharp, vibrant vision, helping you see the world the way it’s meant to be seen.
What Are the Symptoms of Cataracts?
A person who has developed cataracts in one or both eyes may experience some or all of the following visual symptoms when seen in the mirror:
- Difficulty with night vision, especially while driving
- Blurry or cloudy images
- Seeing colors in muted shades, or with a yellowish or brown cast
- Sensitivity to glare, or halos that surround lights at night
- Double vision (in one or both eyes)
- Frequent prescription changes
Types of Cataracts: Understanding the Different Forms and Causes
Most people are familiar with age-related cataracts, typically affecting people over age 60. The American Academy of Ophthalmology estimates that normal cataracts today affect more than 24.4 million Americans age 40 and older and that by age 75, half of all Americans have them. They are the most common cause of blindness in the world, per Prevent Blindness America. However, there are other forms of cataracts, including:
-
Congenital Cataracts: Present at birth or developing within the first year of life, congenital cataracts can sometimes be mild and not affect vision. More severe cases require the same surgical treatment used for adults. These cataracts may also be linked with other birth conditions.
-
Radiation Cataracts: Exposure to certain types and amounts of radiation can lead to cataracts. High doses might cause cataracts within a year or two, while lower doses can cause changes over many years.
-
Secondary Cataracts: These aren’t new cataracts but a clouding of the lens capsule that remains after cataract surgery. Though less common, secondary cataracts can develop months or years after surgery and may require treatment.
-
Traumatic Cataracts: Injuries to the eye, whether recent or long ago, can damage the lens and lead to cataract formation over time.
Cataracts are also classified by the part of the lens they affect:
- Nuclear Cataracts: Form in the center of the lens and often cause a yellow or brown tint to vision.
- Cortical Cataracts: Start at the edges of the lens and gradually move inward, often causing glare or light streaks.
- Posterior Subcapsular Cataracts: Develop at the back of the lens and tend to progress faster, affecting night vision and reading in bright light.
How Do Cataracts Develop?
While no single, definitive cause of cataracts has been determined, researchers have associated many factors with their occurrence. They include:
- Ultra-violet radiation (UV): Primarily from being in the sun too much without protection
- Severe nearsightedness: A condition also known as high myopia
- Genetic links: Traits often identified in family history
- Lifestyle factors: Obesity, smoking, and high alcohol consumption
- Co-morbid conditions: Diabetes and high blood pressure
- HRT: Hormone replacement therapy
- Long-term or overuse of prescribed drugs: Corticosteroid or statin medicines
- Eye injuries: Previous eye surgery, injuries, or ailments to the eyes
Treatment Solutions: Advanced Cataract Lens Options
When we remove your cloudy lens (cataract), we replace it with an intraocular lens (IOL). According to the International Specialist Eye Center, an intraocular lens is a tiny, lightweight, clear plastic disk placed in the eye during cataract surgery. An IOL replaces the focusing power of the eye’s natural lens. Modern IOL options allow us to restore not just clear vision—but also to tailor your vision to your lifestyle needs.
Monofocal IOLs
- Best for single-distance vision: Monofocal lenses are ideal for seeing clearly at one distance—usually far vision.
- Reliable & cost-effective: Typically covered by insurance, they provide clear sight at a chosen distance.
- Glasses may still be needed: You’ll likely need reading or intermediate glasses.
Toric IOLs
- Corrects astigmatism: Designed to fix both cataracts and corneal distortion, delivering sharper distance vision.
- Fewer glasses for distance: Great for patients with astigmatism who want to reduce reliance on distance glasses.
- You may still need them up close: Reading or computer use may still require glasses.
Multifocal / Trifocal / Extended Focus (EDOF) IOLs
- Multiple focal points or a continuous range: Multifocals offer two distances; trifocals add intermediate; EDOF lenses provide a smooth transition from near to far.
- Advanced freedom from glasses: Ideal for active individuals who want minimal use of glasses across all ranges—reading, computer, driving, everything.
- Premium technology: These options cater to modern visual demands, including digital screens and active lifestyles.
Light Adjustable Lens
-
The only IOL that can be customized after surgery — fine-tune your vision as you heal.
-
Adjustments made using light treatments after your eye recovers, giving you precise control over your final vision outcome.
-
Ideal for those seeking maximum accuracy, especially patients with prior refractive surgery like LASIK or PRK.
The right IOL can help you achieve clear, vibrant vision tailored to the way you live — whether you’re reading, driving, working on a computer, or enjoying the outdoors. Our cataract specialists will guide you through your options, considering factors like astigmatism, prior eye surgery, and how much you’d like to reduce your dependence on glasses.
Related content: A Guide to Cataract Surgery Lenses
Cataract Surgery
Most doctors recommend having cataract surgery once the changes in your vision begin to affect your ability to perform your normal daily activities.
Once you’ve made the decision to undergo the procedure, you will be scheduled for outpatient eye surgery by your doctor. On the day of the surgery, you’ll be given Valium or similar medicine to help you relax.
Your surgeon will numb your eye with anesthetic eye drops, dilate your pupil with more drops, and then make a tiny incision in your cornea through which your cloudy lens is removed and a clear artificial lens – called an intraocular lens – is inserted in its place. That lens will remain permanently in your eye. In appropriate cases, the inserted lens can be made to your prescription, which ends the need for corrective eyeglasses or contact lenses post-surgery.
The surgery itself takes only minutes, though prep and aftercare mean you’ll be at the facility for two to three hours. Typically, your eye has a protective shield over it when you are released, which remains in place for a few hours. You’ll be given antibiotic drops to prevent infection and will be advised to use artificial tears to relieve any scratchiness or irritation in the coming days. Patients tend to wear an eye guard at night while their eye heals to prevent accidentally rubbing the eye during sleep.
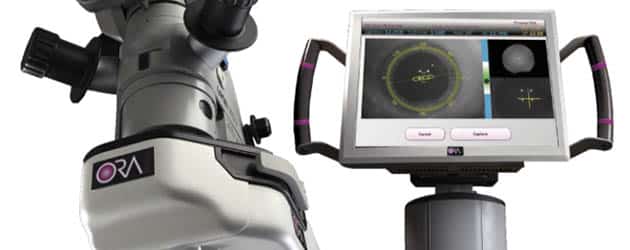
ORA™ Optiwave Analysis: Real-Time Precision for Cataract Surgery
At Barnet Dulaney Perkins Eye Center, we’re committed to providing the most advanced care so you can achieve your best possible vision. That’s why we’re proud to offer ORA™ (Optiwave Refractive Analysis) — an FDA-approved technology that gives our surgeons real-time, precise measurements during cataract surgery.
ORA technology enhances accuracy beyond what’s possible with standard pre-surgery tests. During your procedure, ORA uses a gentle, invisible beam of low-intensity light to measure your eye’s unique optical characteristics. This light reflects back to sensors in the device, allowing your surgeon to fine-tune decisions about your lens implant and astigmatism correction — while you’re on the operating table.
Why Choose ORA?
ORA helps ensure your cataract surgery results are as accurate as possible. It’s especially valuable for:
- Patients who want the most precise outcomes
- Those choosing advanced technology lenses (such as multifocal, trifocal, accommodative, or toric IOLs)
- Patients with astigmatism who want to minimize dependence on glasses
- People who have had prior LASIK or PRK
- Patients undergoing laser-assisted cataract surgery (such as LenSx®)
The Benefits of ORA
- ORA analysis can improve accuracy for any cataract procedure — no matter which lens you select.
- It gives your surgeon a live, detailed map of your eye’s optical system during surgery to guide fine adjustments.
For patients with astigmatism, ORA can enhance the precision of correction, helping reduce the chance you’ll need glasses after surgery.
Take the Next Step Toward Clearer Vision
Cataract surgery can help you rediscover a world of vibrant color and sharp detail. With advanced technologies like ORA and premium lens options, Barnet Dulaney Perkins Eye Center is here to guide you toward your best possible vision.
Schedule your cataract evaluation today — book online or call us. We look forward to helping you see life clearly again.

