
Macular Degeneration Specialists
AGE-RELATED MACULAR DEGENERATION
The retina is a remarkable, delicate sheet of nerve tissue that coats the back of the eye wall and receives signals from light waves. These complex signals of light are transmitted to the brain and interpreted as vision. The retina, then, is like the “film” in the “camera of your eye.” The macula is a small area of the retina responsible for our most precise central vision. The unique properties of the macular portion of the retina allow us to process fine visual details required for tasks like reading a book, recognizing faces, driving, or appreciating leaves on the trees from a distance.
As the eyes age, the macula is increasingly at risk of undergoing some deterioration. Age-related macular degeneration (AMD) is a single term used to describe a host of damaging effects that can develop in the aging macula. The degenerative effect of AMD is due to a combination of age, genetics, and environmental factors (such as oxidizing molecules in the environment and toxins like those found in cigarette smoke). Though AMD actually has a host of sub-types, for purposes of explanation AMD can be distinguished as either dry or wet. This distinction also guides options for therapy.
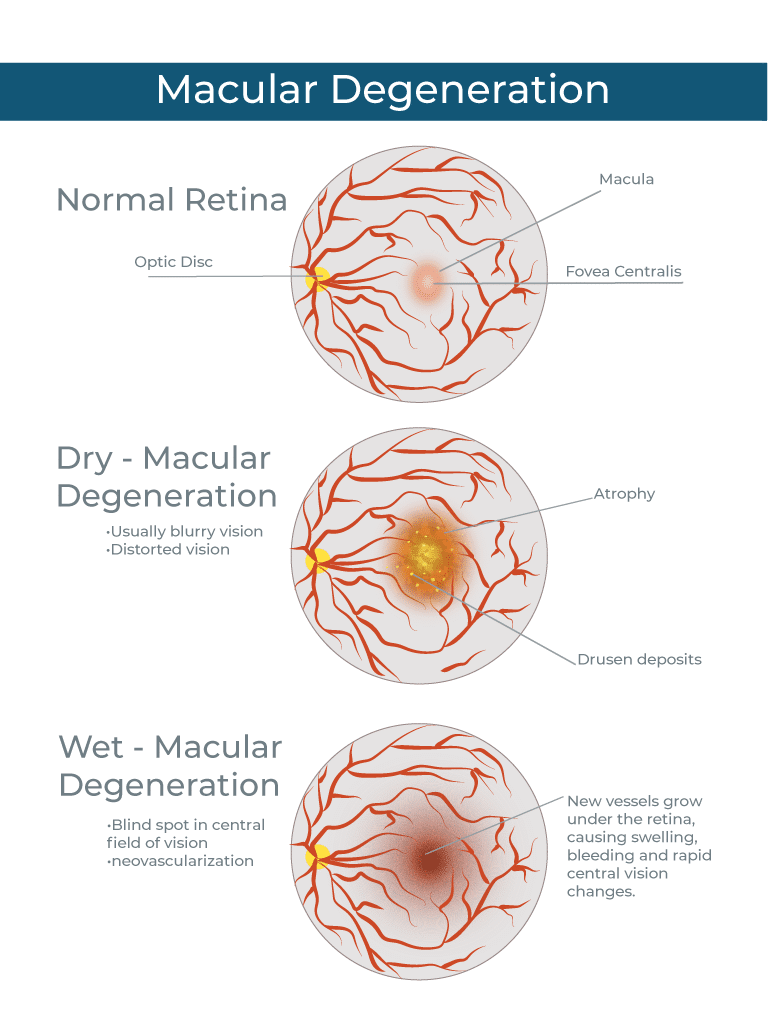
DRY AGE-RELATED MACULAR DEGENERATION (DRY AMD)
Dry AMD accounts for about 90 percent of macular degeneration cases treated by our retina doctors in Phoenix, Tucson, and across Arizona. Dry AMD is caused by the degeneration of pigmented cells in the macula (the retinal pigment epithelium or RPE) and the build-up of waste products in the retina (drusen). The breakdown of the RPE and accumulation of drusen begin to affect the photoreceptors themselves and cause vision loss. When this happens, the patient may recognize that the central vision is increasingly blurry or has areas of distortion. Some patients also notice missing spots in the central vision, or that they require more light than usual to read or see small details.
Changes from dry macular degeneration may be very gradual and may affect one eye more than another. The patient may not notice a distinct change in vision until considerable damage has already occurred. As a result, it is important for patients over age 50 to undergo regular dilated macular examinations to look for macular degeneration. If early AMD changes are present, your retinal doctor will obtain baseline images and carefully monitor your condition. The addition of high-dose anti-oxidants may be prescribed (as per the data from the Age-Related Eye Disease Study, or AREDS). Your doctor may also talk with you about the beneficial role of dietary changes to include more vegetables, fish oils, and berries. These steps may help to prevent progression to the more serious “wet” AMD.
WET AGE-RELATED MACULAR DEGENERATION (WET AMD)
Wet macular degeneration occurs when abnormal, fragile blood vessels form underneath the macular tissue. Because they are not normal vessels, these blood vessels often leak blood and other fluid into the tissues of the macula, forming blisters and cysts of fluid that damage the retina and affect vision. The first symptom of wet macular degeneration often reported is that straight lines appear wavy or that the central vision is ‘blurry.’ Because new and increasingly effective treatment options are now available to manage wet AMD, a patient who is experiencing these symptoms should seek retina evaluation as soon as possible.
If your retinal surgeon confirms a diagnosis of “wet AMD,” there is hope. New medications have been proven very successful at reducing the progression of vision loss from wet AMD. Bevacizumab (Avastin) and ranibizumab are two variations of anti-vascular endothelial growth factor (anti-VEGF) medications that can be administered to treat leaking blood vessels beneath the retina. Injections are given in a series of treatments every 4 to 6 weeks. In over 90% of cases when injections are continued, the vision loss is halted. In 30-40% of cases, some of the vision that had been lost can be restored. Combination therapies involving photodynamic therapy (PDT or “cool laser”) and anti-inflammatory medications may be helpful in some cases.
Our surgeons have also been involved in the study of new medications that are in development. It is anticipated that new treatments may last even longer and have additional efficacy in the treatment of wet AMD.
Get Help Today
If symptoms of retinal diseases are making you uncomfortable and interfering with your daily life, call us. Our doctors across Arizona have the expertise and tools to give you the relief you need.
